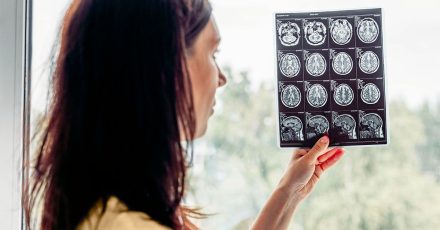
A new Mental Health America report, State of Mental Health in America 2025, finds nearly a quarter of U.S. adults—about 23%, roughly 60 million people—experienced a mental illness in the past year. Overall adult mental health levels were steady from 2021 to 2024, but the report highlights big differences in care and outcomes across states.
Key findings:
– About 23% of adults experienced a mental illness in the past year.
– Youth mental health remains a serious concern: 11% (about 2.8 million) of 12–17-year-olds had a major depressive episode (MDE) affecting functioning in 2024.
– Reports of MDE among youth fell from about 18% in 2023 to 15% in 2024; youth reporting suicidal thoughts dropped from about 12% to 10% in that period.
– Nearly 3 million young people ages 12–17 reported frequent suicidal thoughts in 2024.
– States ranking highest for mental health and services: New York, Hawaii, New Jersey. Lowest: Alabama, Arizona, Nevada.
– Around 27% of adults reported 14 or more days per month when they could not get mental health care due to cost.
– There is roughly one mental health professional for every 320 people in the U.S.
– In 2022–2023, about 1 in 4 adults with any mental illness reported unmet need for care; over 5 million people (~9% of the population) were uninsured.
What this means
The persistence of high prevalence and widespread unmet need suggests the system is not keeping pace with demand. Reduced stigma and greater willingness to seek help may have increased demand, while better integration of services into schools and primary care has expanded access for some. Still, cost, gaps in insurance coverage, provider shortages (especially psychiatrists and psychiatric nurse practitioners), and time or scheduling barriers prevent many people from getting care.
Financial and policy pressures also affect mental health. Cuts to Medicare, Medicaid, and other safety-net programs can restrict services and worsen social determinants of mental health—housing, food security, education, employment, and family supports—that shape brain development and behavioral health.
Practical ways to find help
– Schools: Many schools offer counseling or on-site psychiatric and psychological services for children and teens.
– Primary care: Your primary care provider can screen, offer initial treatment, and refer you to specialists.
– Low-cost options: Look for sliding-scale community clinics, graduate training clinics, pro bono or volunteer services, and community mental health centers.
– Telehealth and integrated care: Telehealth, behavioral health embedded in primary care, and peer support programs can reduce cost and scheduling barriers.
– Peer and community supports: Peer programs, support groups, and local community resources can help when professional services are limited.
A broader approach
Improving population mental health requires attention beyond clinical care. Policies and programs that strengthen employment, housing, education, and family supports are essential to reduce unmet needs and improve outcomes at scale.
If you or someone you know is in immediate danger or having suicidal thoughts, contact emergency services or your local crisis line right away. For non-urgent help, reach out to a primary care provider, local mental health center, school counselor, or the low-cost options listed above.