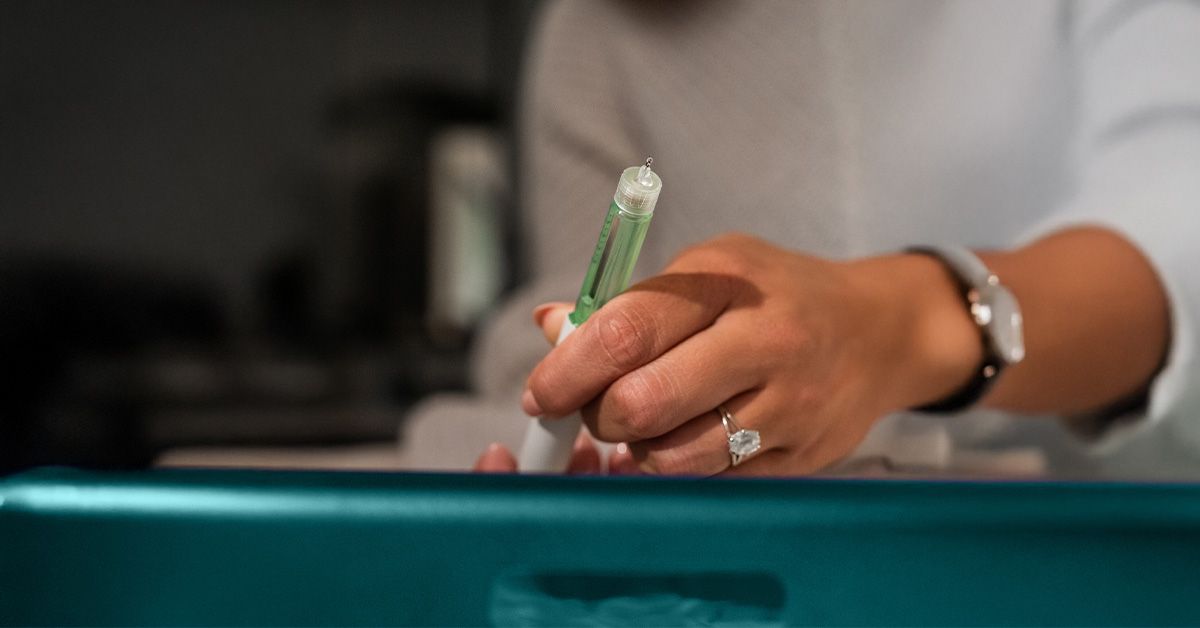
Reports of people on GLP-1 medications being diagnosed with scurvy have increased recently. The link isn’t that the drugs directly cause vitamin C loss, but that many GLP-1s reduce appetite and slow gastric emptying, which can lead to markedly lower food intake and poorer intake of vitamin C–rich foods like fruits and vegetables.
A July 21, 2025 BMJ opinion by Ellen Fallows warned that prescribing GLP-1s to patients who already eat nutrient-poor diets can reveal or worsen malnutrition. She noted that people with obesity can be “overnourished” in calories yet undernourished in key vitamins and minerals, and that combining an unhealthy diet with calorie restriction can produce serious deficiencies. Fallows also pointed out that other factors—like GI inflammation or medications such as metformin—can contribute to nutrient shortfalls. Reported deficiencies among GLP-1 users include vitamin C, thiamine, and magnesium. She advised that care for patients on GLP-1 agonists should go beyond generic dietary advice and include nutritional assessment before and during treatment.
Registered dietitian Fiorella DiCarlo explains that GLP-1s cause early satiety and slower motility, so some patients unintentionally eat only 600–1,000 calories per day and miss essential nutrients. People often avoid fruits and vegetables because of reduced appetite or aversion to acidic or raw foods, and may substitute lower-nutrient options like toast, crackers, or processed foods to manage nausea and other GI symptoms. Over time this can cause vitamin C deficiency, which presents with symptoms such as easy bruising, bleeding gums, poor wound healing, and weakened blood vessels—classic signs of scurvy. Fortunately, scurvy is reversible with appropriate supplementation (for example, a daily multivitamin or 100–200 mg vitamin C) and diet correction.
How to reduce risk while taking GLP-1s
– Have nutrition assessed before starting therapy and monitor status during treatment, especially if you have a history of poor diet.
– Work with a Registered Dietitian to plan meals that meet nutrient needs despite reduced appetite.
– Prioritize protein and consume meals on a schedule to help maintain intake. Start meals with protein, then vegetables, so vitamin- and fiber-rich foods are eaten earlier when you feel less full.
– Include fiber from fruits, vegetables, and legumes to help counter constipation from slowed motility.
– Choose high-protein snacks such as low-fat yogurt, cottage cheese, or kefir to maintain protein, calcium, and vitamin D intake.
– Stay hydrated to reduce dehydration risk.
– Consider targeted supplements (multivitamin or vitamin C) if dietary intake is insufficient; discuss dosing with your clinician or dietitian.
– Watch for symptoms of deficiency—bleeding gums, easy bruising, slow-healing wounds, unusual fatigue—and seek medical evaluation if they appear.
Summary
GLP-1 medications can improve weight and metabolic measures, but because they reduce appetite and slow gastric emptying, they can increase the risk of malnutrition and nutrient deficiencies—even scurvy—if dietary intake of key foods falls too low. Proper pre-treatment assessment, ongoing monitoring, meal planning with a dietitian, and supplementation when needed can prevent and reverse deficiencies while allowing effective use of these drugs.