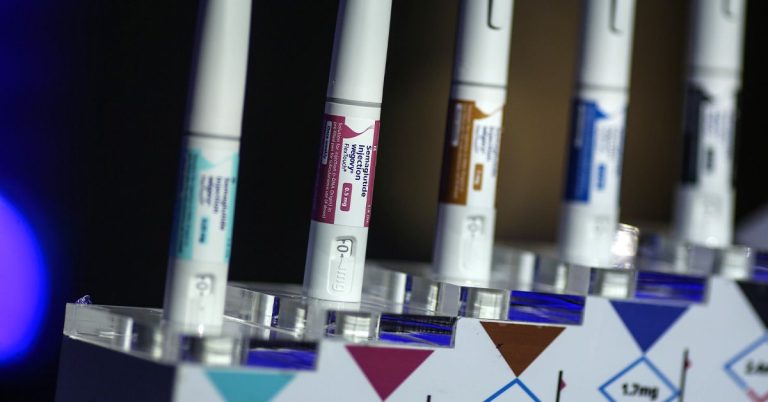
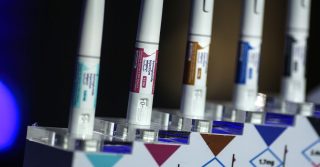
A vomiting disorder linked to chronic cannabis use is rising sharply in the United States. A large, retrospective analysis of emergency department (ED) visits published in JAMA Network Open found that cases identified as cannabinoid hyperemesis syndrome (CHS) increased fivefold between 2016 and 2022, peaking during the COVID-19 pandemic.
The study’s lead investigator, James A. Swartz, PhD, and colleagues analyzed more than 188 million ED visits—about 85% of U.S. ED visits. Because CHS did not have a dedicated ICD code at the time (it received one in 2025), researchers used a proxy: concurrent diagnoses of cannabis use disorder (CUD) and cyclical vomiting. Using that definition, CHS rose from 4.4 per 100,000 visits in 2016 to 22.3 per 100,000 in 2022, with a peak of 33.1 per 100,000 in 2020.
Young adults 18–25 were disproportionately affected, with a roughly 3.5-fold higher likelihood of receiving a CHS diagnosis than older adults. Notably, CHS cases increased while general cyclical vomiting declined, suggesting a cannabis-specific trend rather than a broad rise in vomiting disorders.
CHS, sometimes called “scromiting” (a blend of “screaming” and “vomiting”), typically progresses through two phases. The prodromal phase can last months or years and features increasing nausea, abdominal discomfort, and fear of vomiting without actual vomiting. The hyperemetic phase involves recurrent, often prolonged bouts of nausea and vomiting, abdominal pain, weight loss, and a compulsive need for hot showers or baths, which some patients find temporarily soothing.
CHS risk rises with chronic, especially daily, cannabis use. Experts point to expanding legalization, wider availability and variety of products, and higher-potency cannabis as likely contributors, though the precise mechanisms remain unclear. CHS was first described in Australia in 2004 and has likely been underrecognized or misdiagnosed, so part of the observed increase could reflect improved recognition by clinicians as well as a real rise in cases.
Prevention and management
– Quitting cannabis is considered the cornerstone of prevention and treatment; cessation is the clearest way to avoid recurrence. Whether reduced or intermittent use reliably prevents CHS recurrence is unknown.
– For people who use cannabis and want to lower risk, clinicians recommend avoiding very high-potency products such as wax, dabs, and shatter, and being mindful of THC content. Some experts suggest most people do not need more than about 25% THC in smoked products and to reduce total daily THC intake.
– If prodromal warning signs (increasing nausea or abdominal discomfort) appear, taking a break or cutting back to see if symptoms remit is advisable.
Study limitations include reliance on a proxy diagnosis because of the lack of an ICD code at the time, and the inability to definitively determine whether the rise reflects more cases or better recognition. Swartz and other experts say it’s likely a mix of both and call for further detailed studies to clarify causes, risks, and effective prevention strategies.